Fungal Toenails
Fungal toenails, medically known as onychomycosis, are a persistent infection caused by dermatophytes; microscopic organisms that feed on keratin, the primary protein in your nails, skin, and hair. Affecting up to 20% of the population, nail fungus is notoriously difficult to treat because the fungi reside not just on the surface, but within and beneath the nail plate.
Onychomycosis
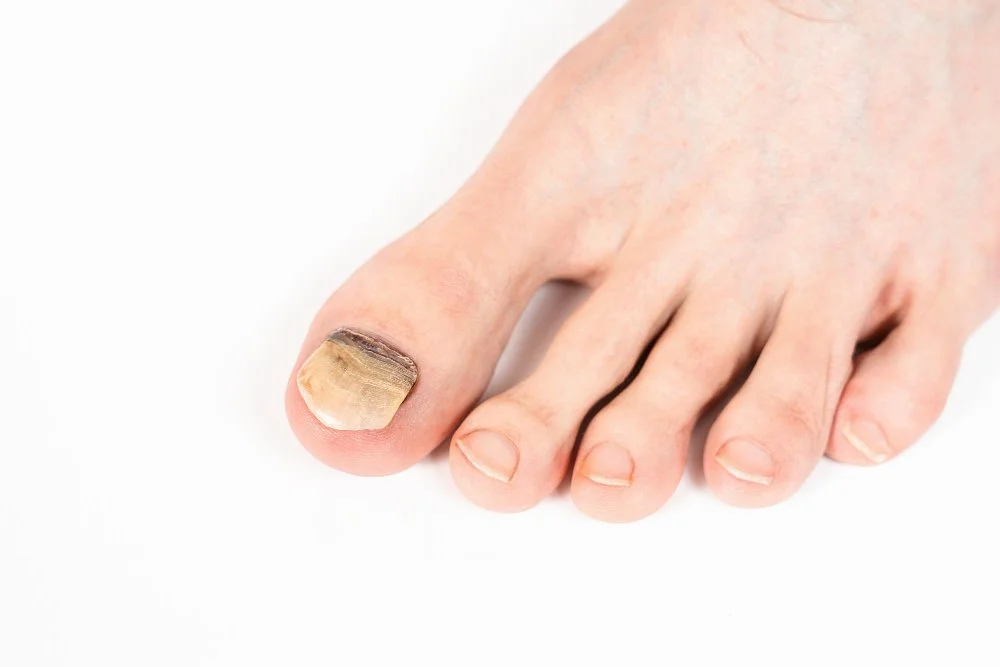

Symptoms
Yellow, white, or greenish discoloration; thickening of the nail plate; brittle or crumbling edges; distorted nail shape; and an unpleasant odor caused by fungal debris trapped under the nail.
Treatment
Topical Antifungals, Oral Medications, Professional Debridement, Total Nail Avulsion (Surgical).
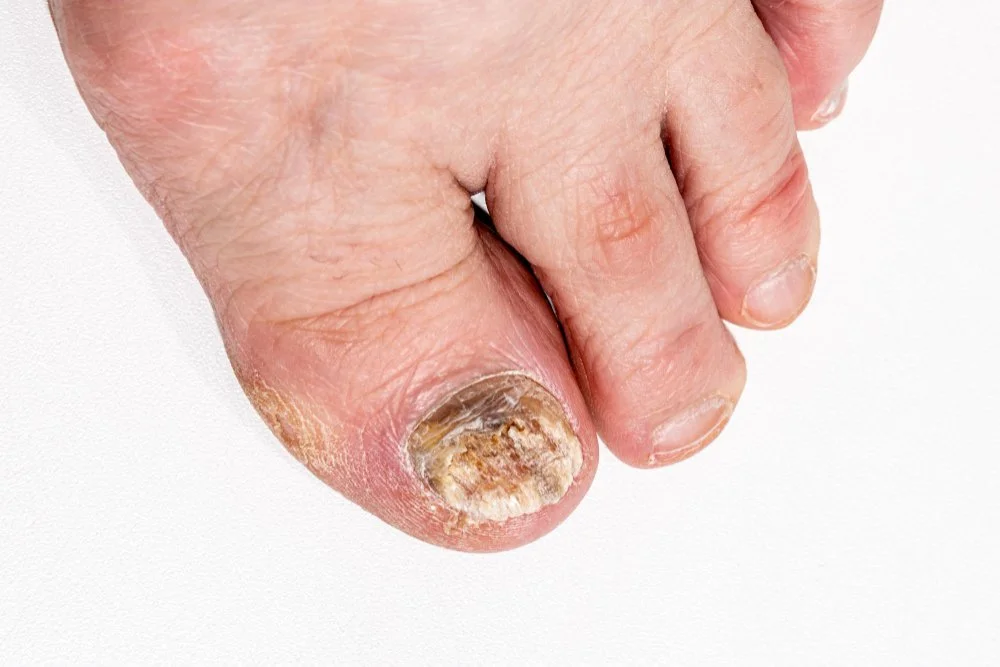
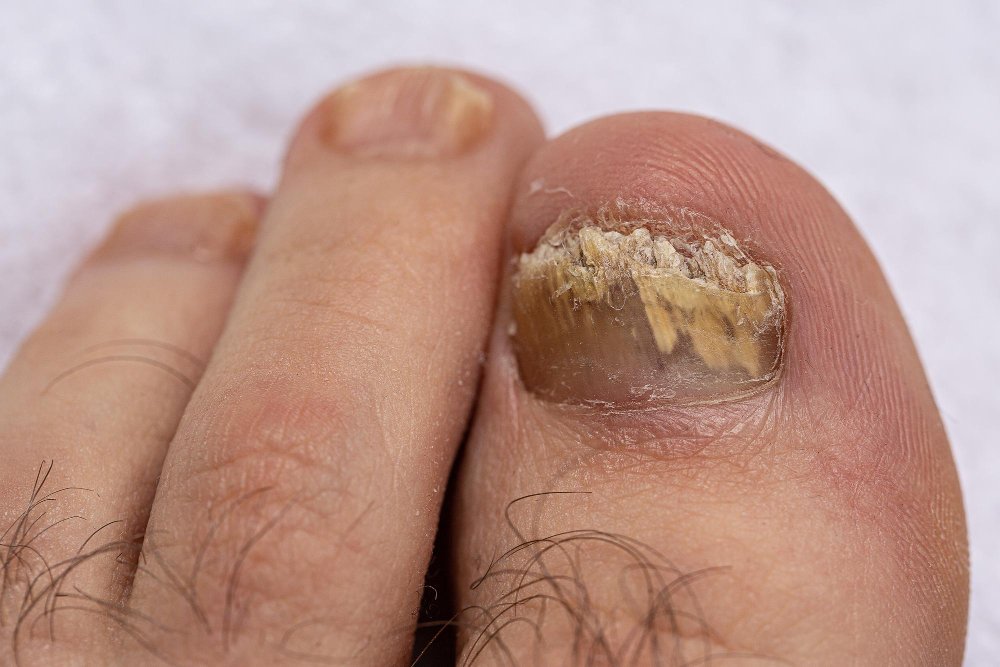
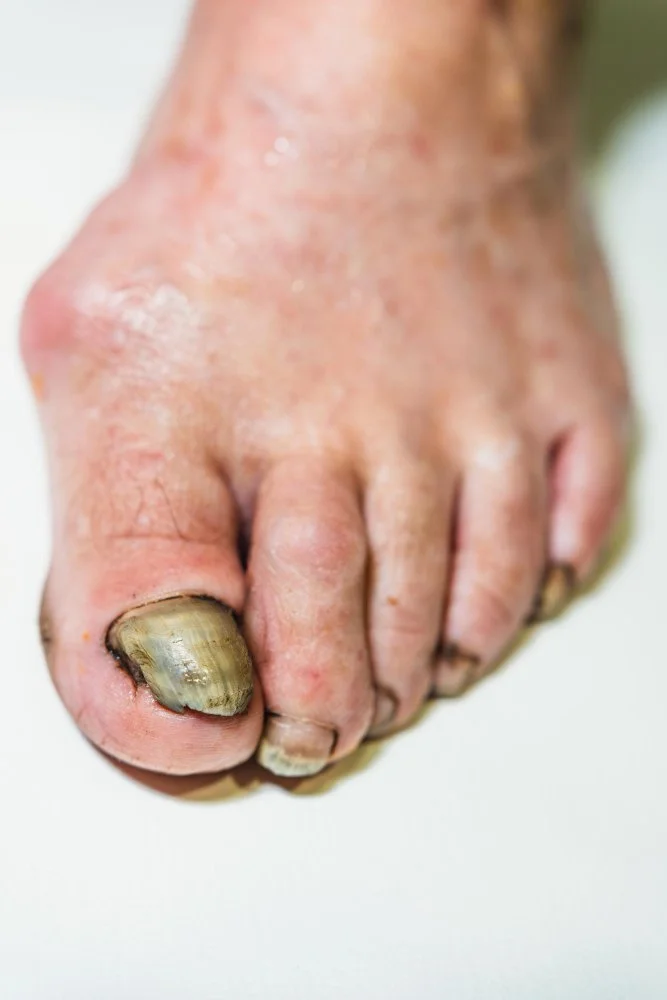
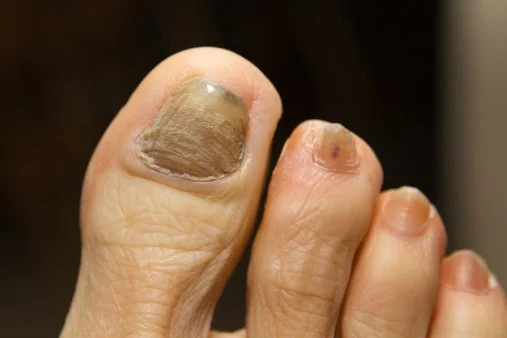
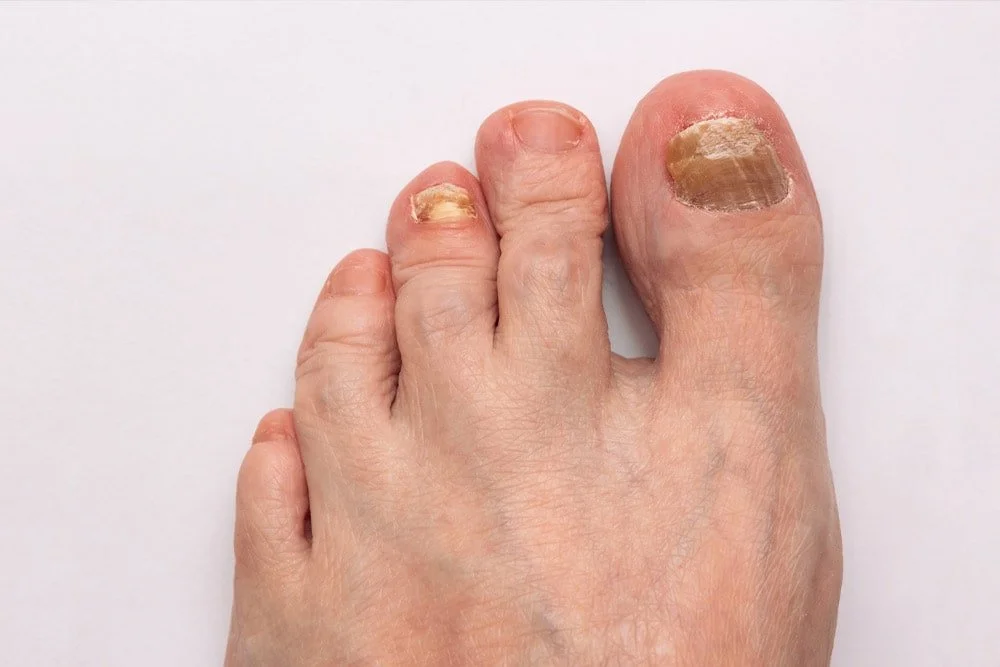
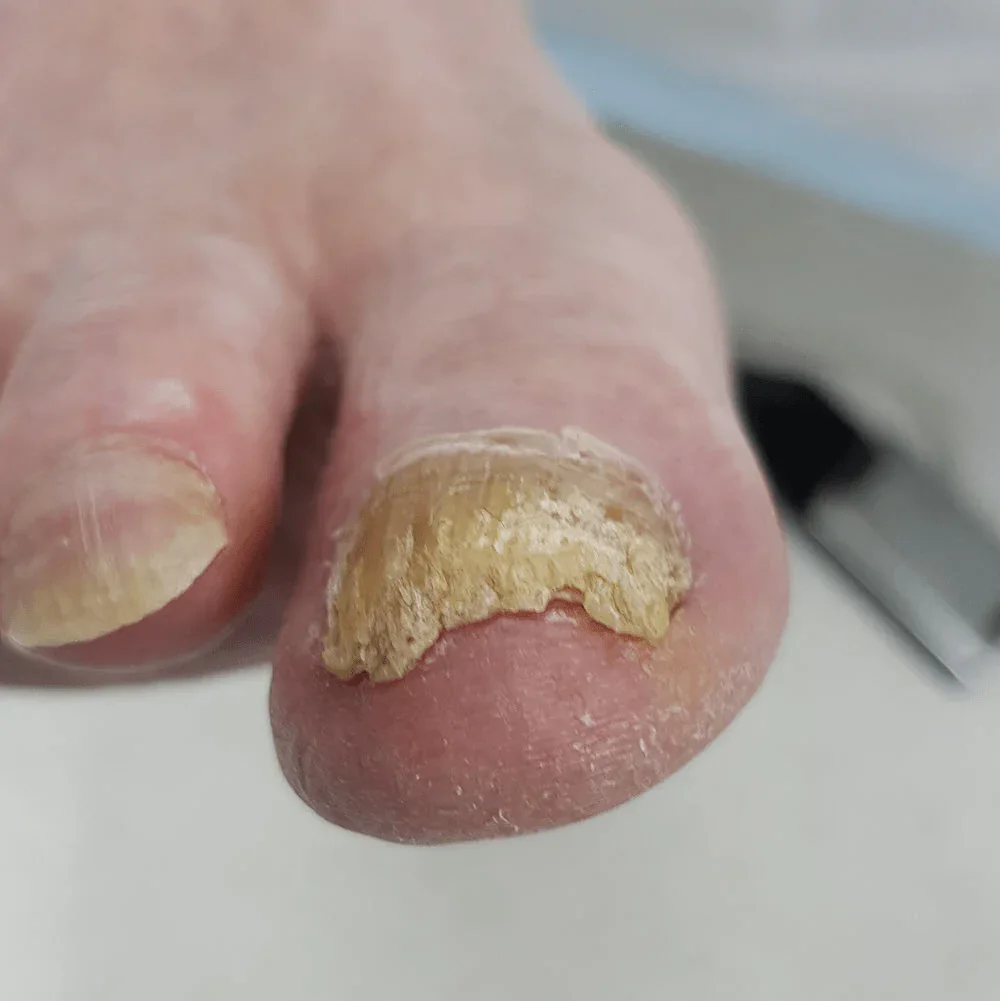
What are Fungal Toenails?
Onychomycosis occurs when fungal spores find their way into the nail bed, often through a microscopic separation between the nail and the skin. Once established, the fungus "digests" the keratin, causing the nail to lose its transparency and become opaque and brittle. Because toenails grow slowly, the infection can remain for years, acting as a reservoir that can spread to the skin (Athlete's Foot) or to other people through shared showers and unsterilized pedicure tools.
What can cause Fungal Toenails?
Fungi thrive in environments that are dark, warm, and moist. Common risk factors include:
Footwear Environment: Wearing non-breathable shoes or damp socks for long periods creates a "greenhouse effect" for fungal growth.
Trauma: A stubbed toe or repetitive "micro-trauma" from tight shoes can lift the nail slightly, allowing spores to enter.
Public Exposure: Walking barefoot in gym locker rooms, public pools, or using contaminated tools at nail salons.
Age and Health: Reduced blood circulation, diabetes, or a weakened immune system can make it harder for the body to fight off fungal invaders.
What are the symptoms of Fungal Toenails?
Discoloration: The nail may turn white, yellow, or even brown/black as the infection progresses.
Hyperkeratosis: A buildup of chalky, crumbly debris under the nail that causes it to lift away from the toe.
Texture Changes: The nail plate becomes "ragged" or flaky and may eventually become so thick that it is painful to wear shoes.
Odor: A distinct, musty smell often accompanies the removal of socks or the trimming of infected nails.
How do you treat Fungal Toenails?
Because the nail acts as a protective shield for the fungus, we use multi-layered treatment strategies:
Professional Debridement: Every 6–8 weeks, our foot specialists use clinical drills to thin out the infected nail. This "de-bulking" reduces pressure and allows topical medications to reach the underlying fungus more effectively.
Oral Medications: For deep-rooted infections, oral antifungals are the "gold standard." They treat the fungus from the inside out, though they require monitoring of liver function via blood tests.
Surgical Nail Removal: In severe or resistant cases, we can safely remove the entire nail under local anesthetic. This eliminates the primary fungal load and allows us to treat the nail bed directly as a new, healthy nail grows in.
How can I prevent Fungal Toenails?
Prevention starts with moisture management and vigilance. Always wear moisture-wicking socks and allow your shoes to dry for at least 24 hours between uses. Utilizing a UV shoe sanitizer can help kill dormant spores inside your footwear. When visiting nail salons, ensure they use high-level sterilization (autoclaves) or bring your own tools. If you notice even a small spot of white or yellow on your nail, seek a professional assessment immediately—treating a small infection is significantly faster and easier than treating a fully thickened, crumbly nail.
Stop managing discomfort and start your recovery.
Book an appointment today and get a comprehensive assessment.
