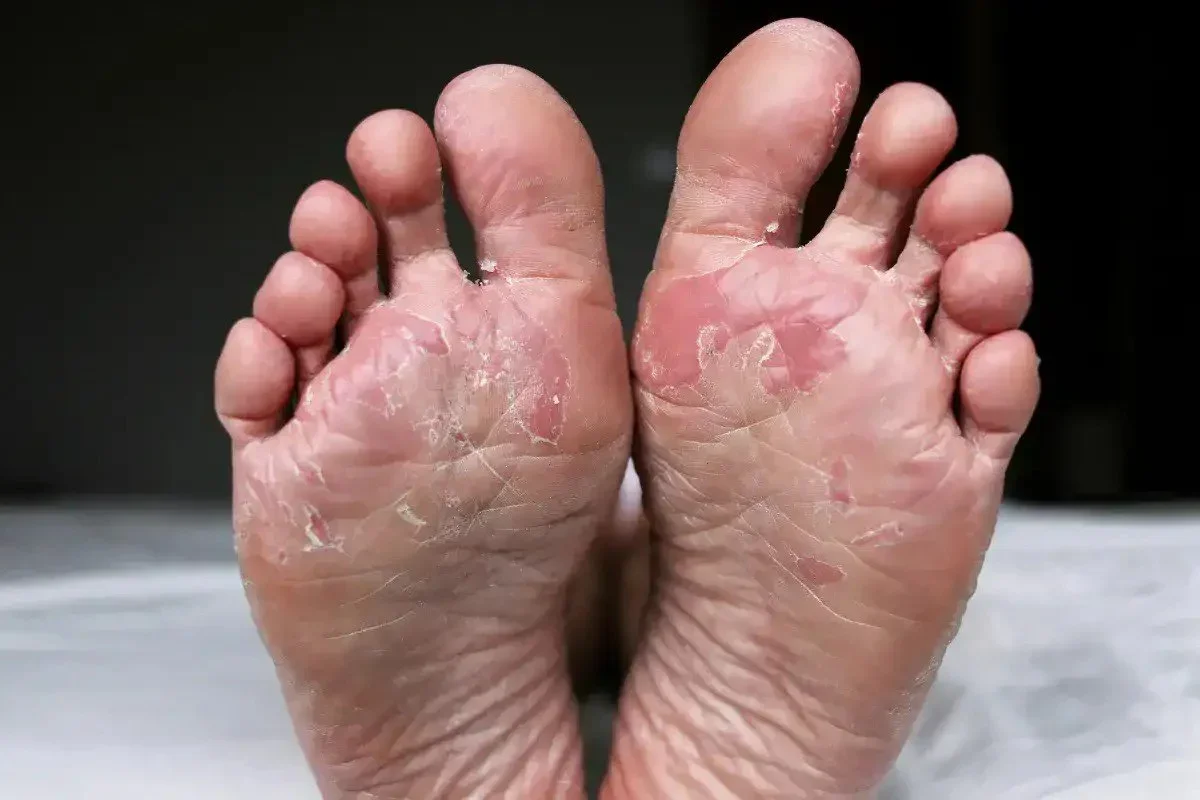
Athlete’s Foot
Athlete’s foot is a common and contagious fungal infection of the skin on the feet. Despite its name, anyone exposed to the causative fungi can develop the condition. The fungi responsible, known as dermatophytes, thrive in warm, damp, and dark environments, making the inside of a shoe the perfect breeding ground. If left untreated, the infection can become chronic, lead to painful skin fissures, or spread to the toenails, resulting in a nail infection.
Tinea Pedis
Symptoms
Red, itchy, or stinging skin; flaking or peeling, especially between the toes; small blisters; unpleasant foot odor; and cracked skin (fissures) that may bleed or weep.
Treatment
Topical Antifungal Therapy, Prescription Oral Medications, Clinical Foot Hygiene Education, Antimicrobial Shoe Sprays.
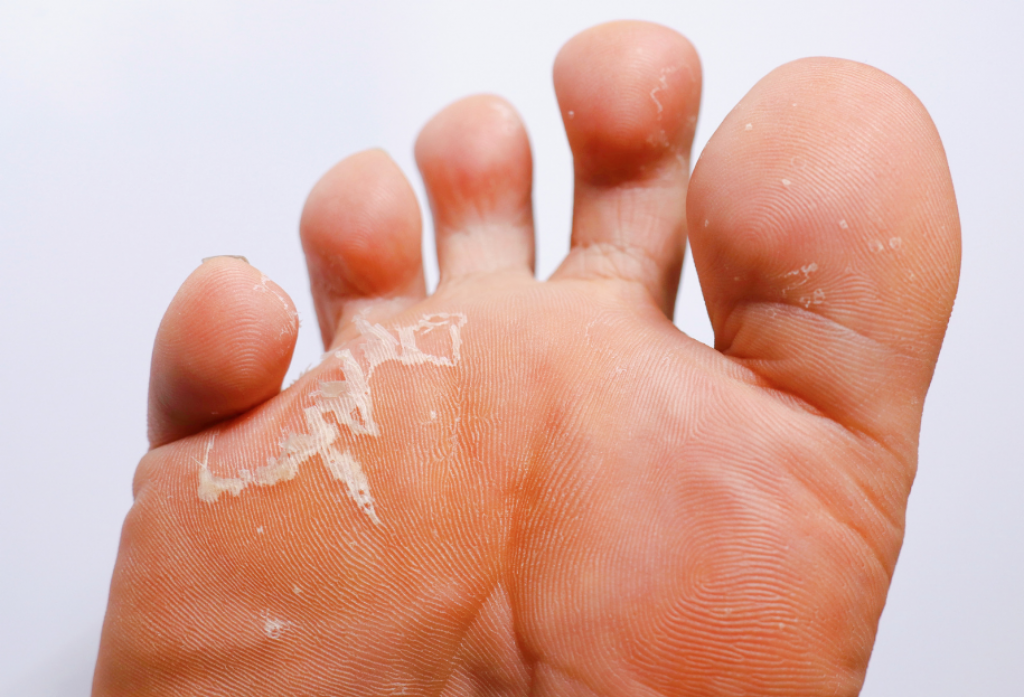
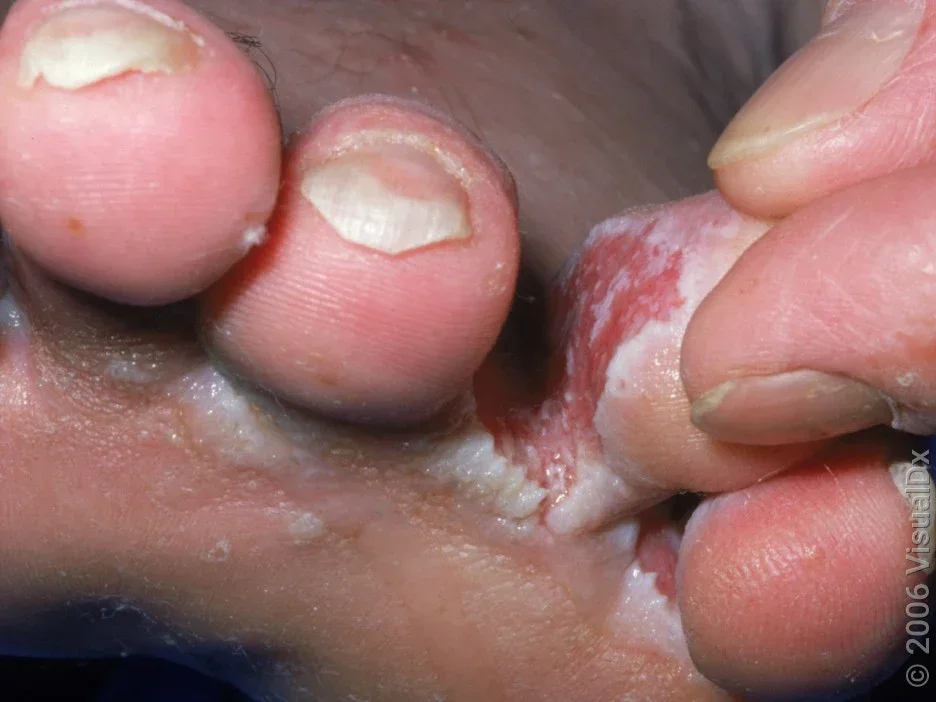
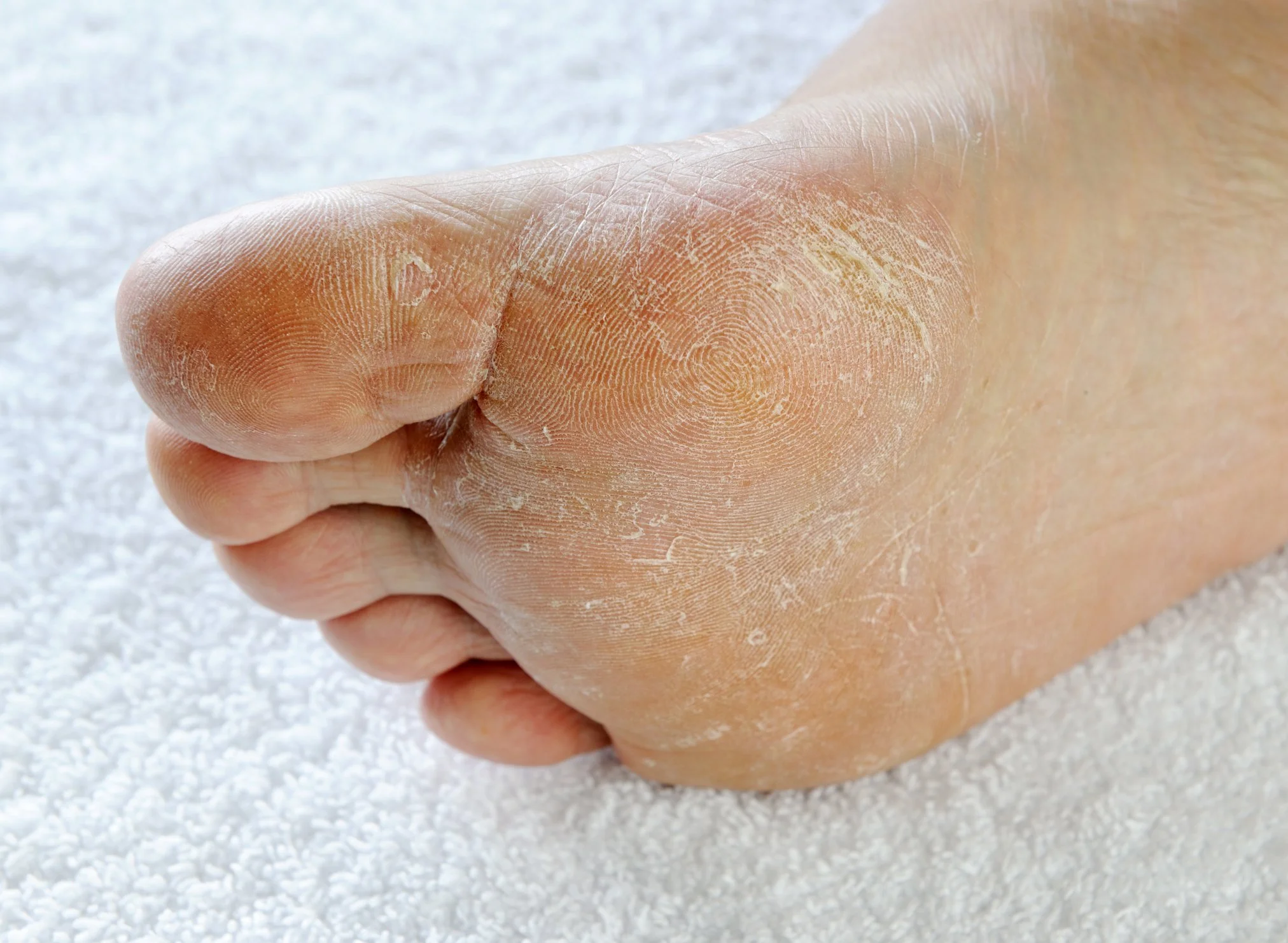
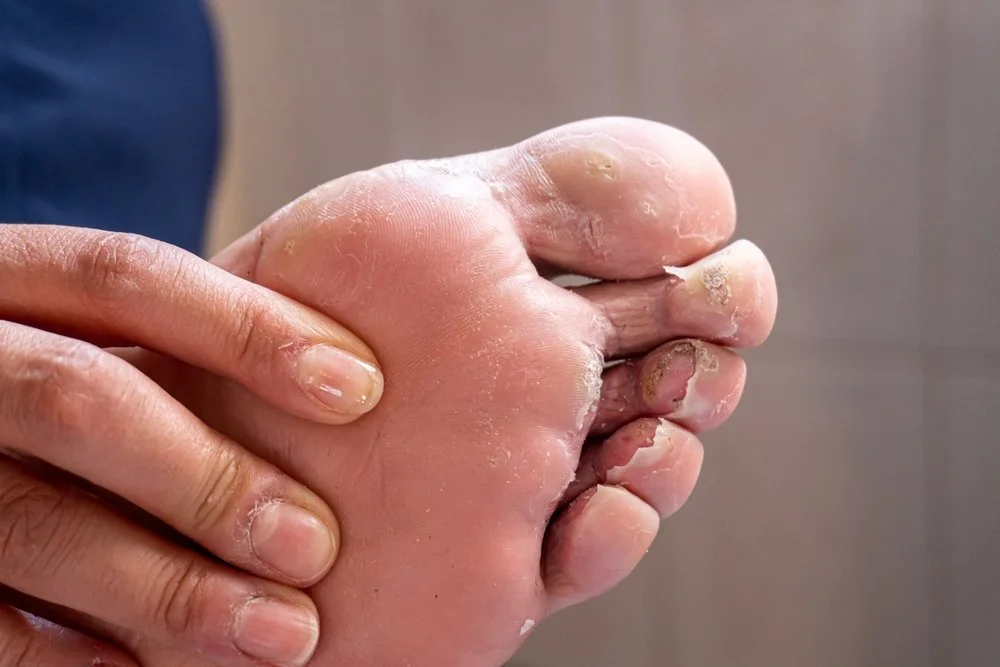
What is Athlete’s Foot?
Athlete’s foot, or Tinea Pedis, is a dermatological infection where fungi invade the outer layer of the skin and feed on keratin. The infection typically manifests in three ways: Interdigital, which occurs between the toes (usually the fourth and fifth); Moccasin, which affects the soles and sides of the feet with dry, silvery scaling; and Vesicular, which presents as sudden outbreaks of fluid-filled blisters. Because the fungi can survive on surfaces like gym floors and inside footwear, the infection is easily transmitted and often recurs if the environment is not properly managed.
What can cause Athlete’s Foot?
At Active Arches, we identify several environmental and biological factors that contribute to fungal growth:
Moist Environments: Keeping feet in wet socks or non-breathable shoes for extended periods creates the humidity fungi need to multiply.
Hyperhidrosis: Excessive sweating of the feet provides a constant moisture source for the infection.
Public Exposure: Walking barefoot in high-traffic, damp areas such as swimming pools, communal showers, and locker rooms.
Compromised Skin Barrier: Tiny cuts, abrasions, or soggy skin (maceration) allow the fungi to penetrate deep into the epidermis.
Poor Foot Hygiene: Failing to wash feet daily or re-wearing damp, unwashed socks.
What are the symptoms of Athlete’s Foot?
Persistent Itching: A hallmark sign, often most intense immediately after removing shoes and socks.
Maceration: Soft, white, "soggy" skin between the toes that may peel away to reveal red, raw tissue underneath.
Scaling and Redness: A dry, scaly rash that can be mistaken for dry skin or eczema but does not respond to standard moisturizers.
Foul Odor: A byproduct of the fungi and bacteria breaking down skin cells and sweat.
Burning and Stinging: Especially prevalent when the skin begins to crack or develop deep fissures.
How do you treat Athlete’s Foot?
Our clinical approach focuses on eliminating the fungi while drying out the environment:
Topical Antifungals: We prescribe clinical-strength antifungal creams, sprays, or powders that are more potent than over-the-counter varieties.
Oral Medication: For severe or "moccasin-type" infections that are resistant to topical creams, a course of oral antifungal medication may be necessary.
Hygiene Protocols: We provide specific instructions on "foot drying" techniques and the use of astringents to reduce excessive sweating.
Footwear Disinfection: We recommend treating all current footwear with antifungal sprays or UV light sanitizers to prevent re-infection from dormant spores.
How can I prevent Athlete’s Foot?
Prevention is centered on moisture control and protection. Always dry your feet thoroughly after bathing, paying special attention to the spaces between the toes. Wear moisture-wicking socks made of synthetic blends or merino wool rather than cotton, which traps moisture. Use flip-flops in all public wet areas, and rotate your shoes daily to allow them at least 24 hours to dry out completely. If you are prone to infections, using an antifungal powder daily can help keep the skin surface hostile to fungal growth.
Stop managing discomfort and start your recovery.
Book an appointment today and get a comprehensive assessment.