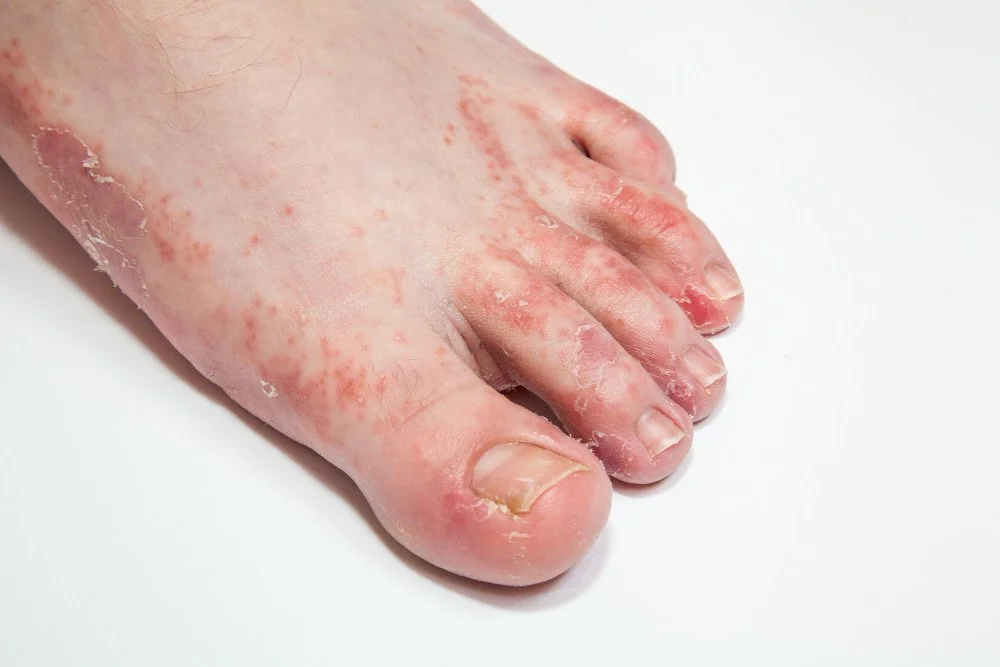
Itchy, Peeling and Rough Skin
Psoriasis and eczema are both inflammatory skin conditions that can cause significant discomfort, but they stem from different biological processes. While Psoriasis is driven by an overactive immune system that accelerates skin cell production, Eczema is often a result of a hypersensitive reaction to environmental triggers or a weakened skin barrier. On the feet, these conditions can look remarkably similar, leading to cracked heels, intense itching, and localized pain that interferes with daily mobility.
Psoriasis and Eczema
Symptoms
Thick patches of red, inflamed skin; silvery-white scales or flakes; deep, painful skin cracks (fissures); itching or burning sensations; and occasionally, small pus-filled blisters (pustular psoriasis).
Treatment
Topical Corticosteroids, Urea-Based Emollients, Light Therapy, Oral Retinoids, Biologic Therapy, Clinical Foot Care.
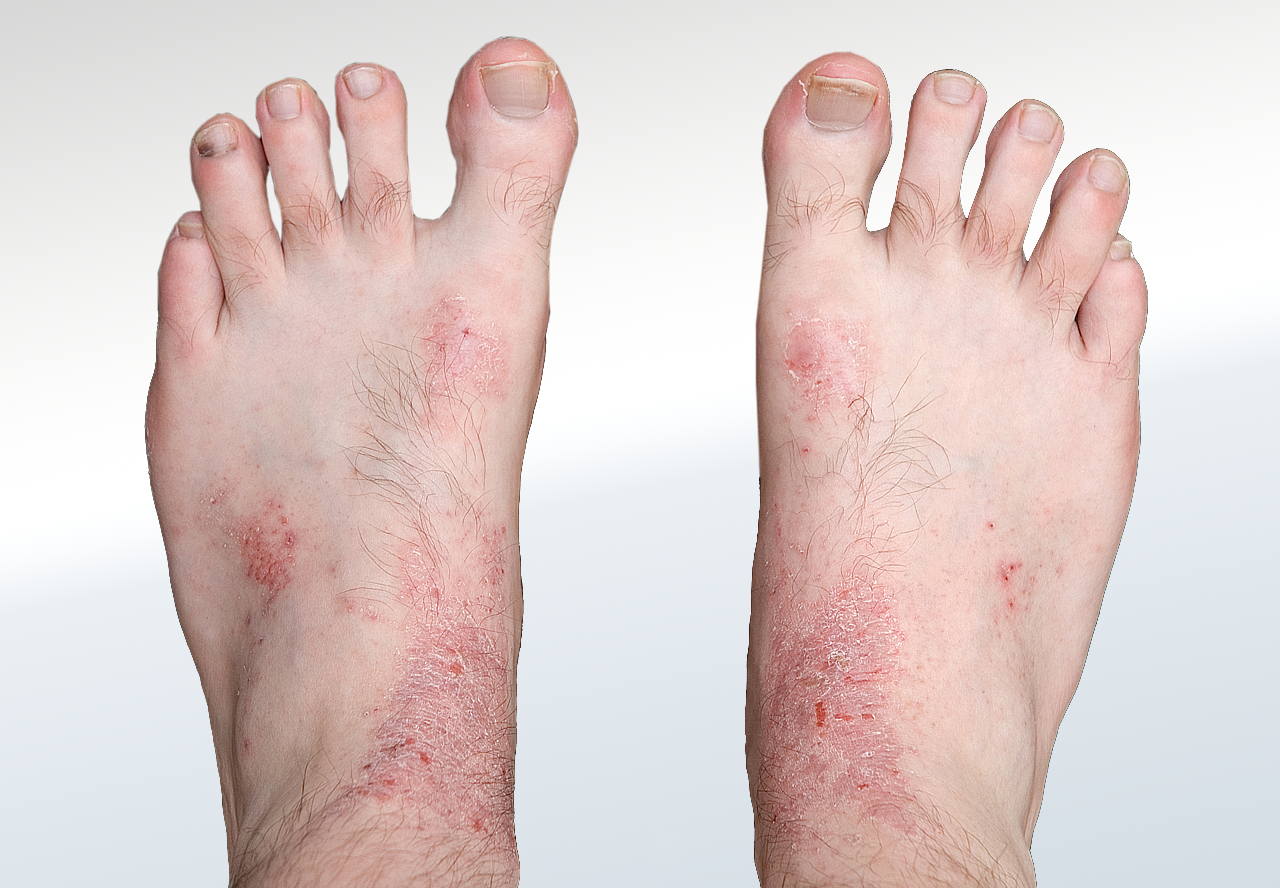
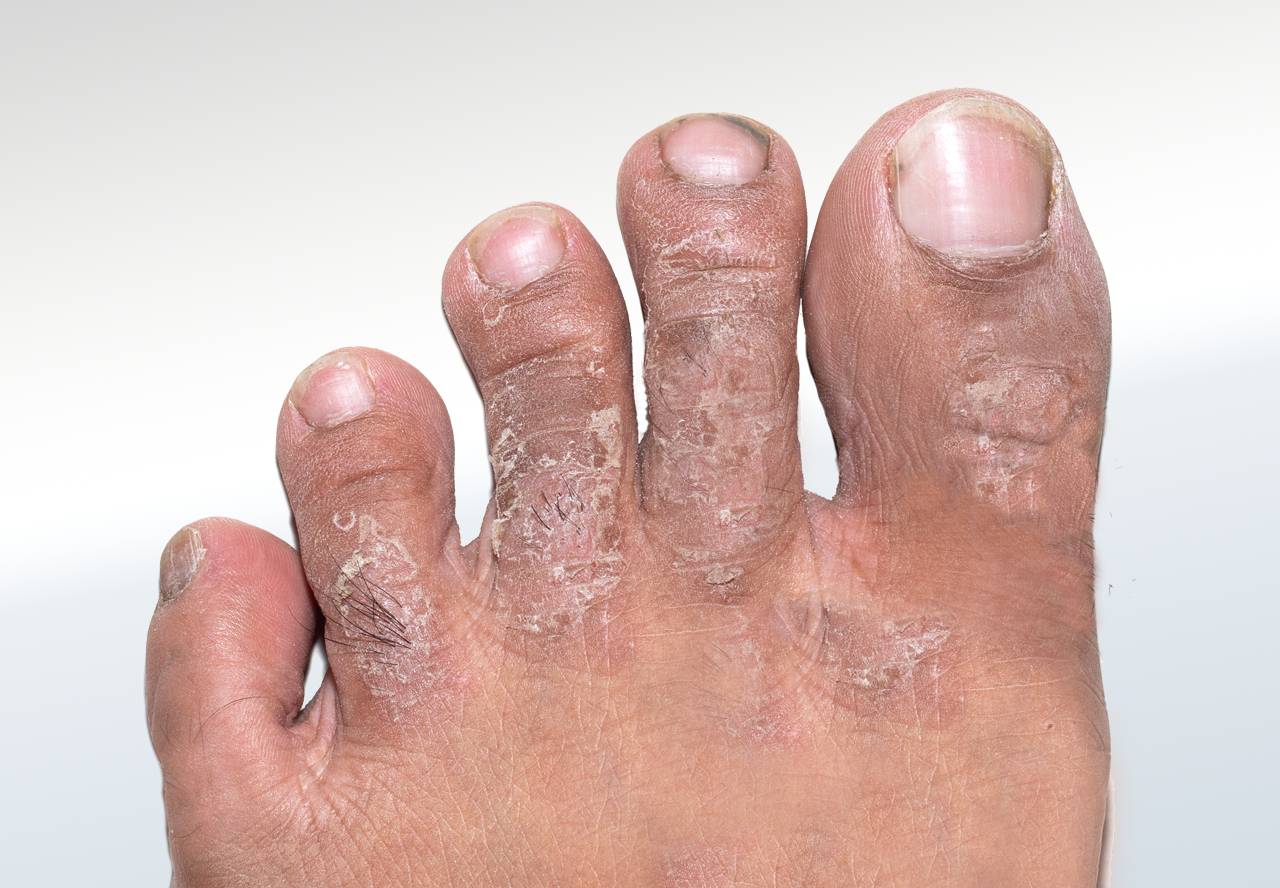
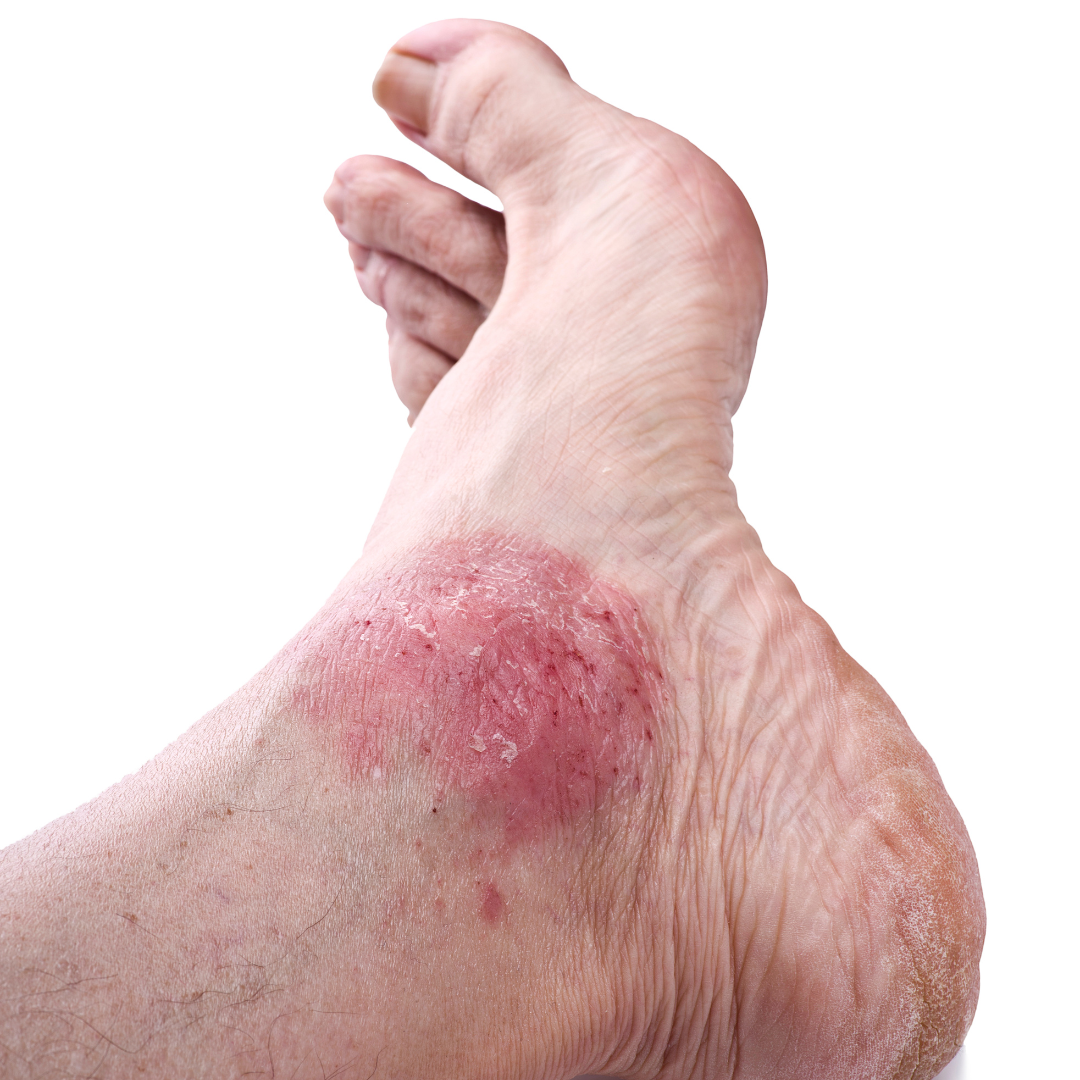
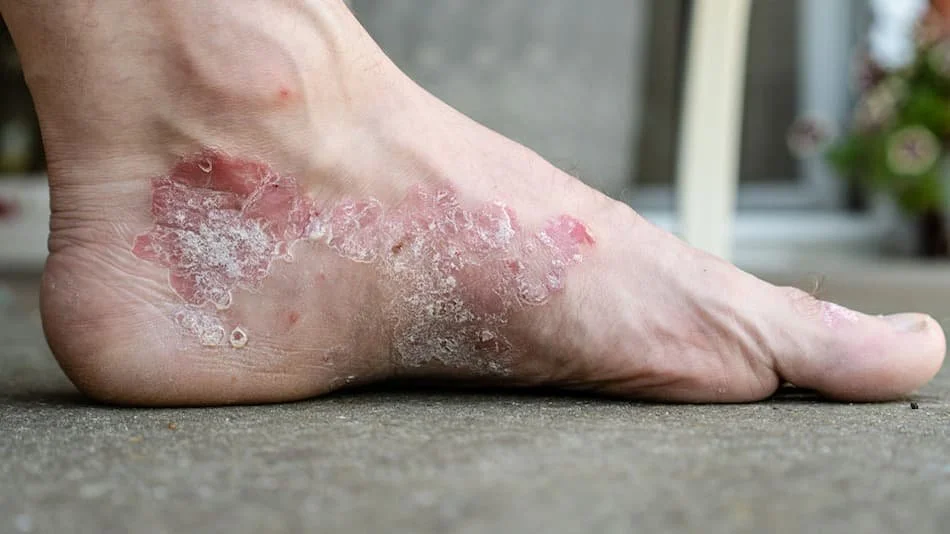
What are Psoriasis and Eczema?
Psoriasis (Palmoplantar) occurs when the immune system mistakes healthy skin cells for invaders, causing skin cells to replicate in days rather than a month. These excess cells pile up, forming thick, silvery "plaques" that can make the soles of the feet feel like they are "too tight" or prone to splitting.
Eczema (Dermatitis), often appearing as "Dyshidrotic Eczema" on the feet, causes tiny, deep-seated blisters and intense itching. It is frequently triggered by a breakdown in the skin’s natural barrier, allowing allergens or irritants to cause a flare-up of red, inflamed, and sometimes weeping skin.
What can cause these skin flares?
Immune System Dysfunction: Both conditions involve an inappropriate immune response, though psoriasis is specifically classified as autoimmune.
Barrier Deficiencies: In eczema, the skin lacks the necessary proteins (like filaggrin) to hold in moisture, making it hypersensitive to socks, shoe materials, or sweat.
Environmental Triggers: High stress, skin injuries (the "Koebner phenomenon"), and contact with harsh chemicals or detergents can activate both conditions.
Weather Extremes: Cold, dry Etobicoke winters strip the skin of essential oils, making both psoriatic plaques and eczema patches brittle and prone to bleeding.
What are the symptoms to look for?
While both conditions cause irritation, psoriasis typically presents with well-defined, silvery-white scales, whereas eczema tends to be more patchy and red, often appearing "wet" or crusty if blisters have surfaced. The nature of the discomfort also differs; eczema is often described as an unbearable itch that leads to a scratch-itch cycle, while psoriasis may feel more like a sore, burning sensation. Additionally, psoriasis frequently affects the toenails—causing small dents called "pitting" or yellowish "oil drop" spots—which is a sign rarely seen in eczema. Because both conditions cause the skin to crack, they create "portals of entry" for bacteria, which can lead to secondary infections characterized by swelling, warmth, or cellulitis.
How do you treat Psoriasis and Eczema?
While there is no permanent cure for these chronic conditions, our goal is to achieve "clearance" and prevent future flares:
Customized Topical Therapy: We prescribe medical-grade corticosteroids to quiet inflammation and Vitamin D analogues to slow down the rapid cell turnover seen in psoriasis.
Keratolytic Debridement: For thick, painful plaques or callused eczema, our specialists safely debride the dead skin. We then apply clinical-grade urea to "soften" the area, allowing medications to reach the living tissue beneath.
Barrier Restoration: For eczema patients, we focus on "sealing" the skin with ceramide-dominant emollients to replace the lipids the skin is failing to produce on its own.
Fissure Management: We treat deep cracks in the heels using medical adhesives or specialized dressings to promote rapid closing and prevent infection.
How can I prevent Psoriasis flares?
Managing inflammatory skin is about proactive maintenance and moisture retention. Regularly applying thick, fragrance-free emollients immediately after bathing helps lock in hydration and keeps the skin supple. It is also beneficial to wear moisture-wicking socks, such as those made from bamboo or merino wool, to prevent sweat from irritating a compromised skin barrier. Most importantly, avoid the temptation to self-diagnose with over-the-counter anti-fungal creams, as these can often worsen an inflammatory flare. A professional assessment at Active Arches ensures you aren't treating an immune-based condition with the wrong medication, helping you maintain a healthy foundation for every step.
Stop managing discomfort and start your recovery.
Book an appointment today and get a comprehensive assessment.