Diabetic Foot Care
Diabetes can significantly impair the health of the lower extremities by affecting the nervous and circulatory systems. Over time, high blood sugar levels can lead to nerve damage and poor blood flow, making the feet highly susceptible to infections and slow-healing wounds.
Diabetes
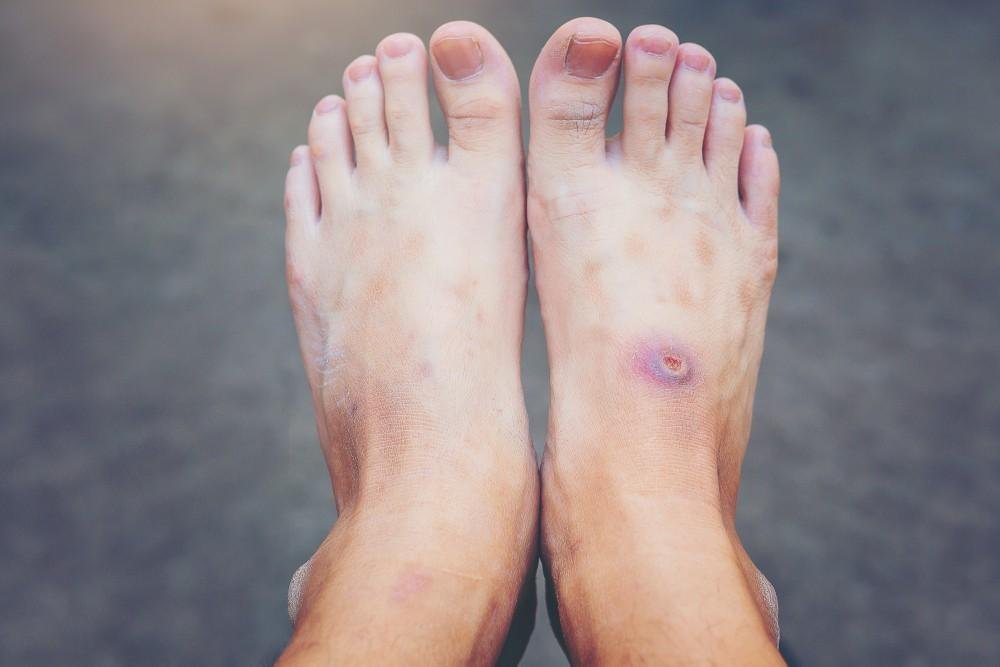

Symptoms
Loss of sensation (numbness); tingling or burning; difficulty reaching or seeing the feet for self-care; thickened toenails; and persistent hard skin or calluses.
Treatment
Neurovascular Assessment, Medical Nail Debridement, Sharp Debridement of Calluses, Wound Care, Custom Orthotics
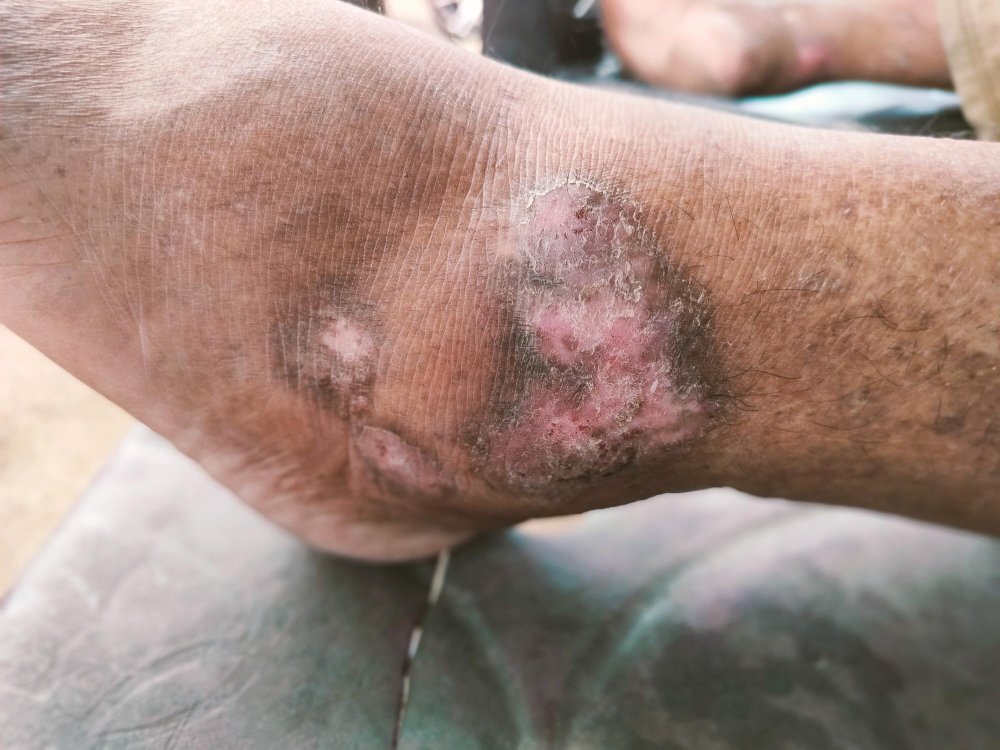
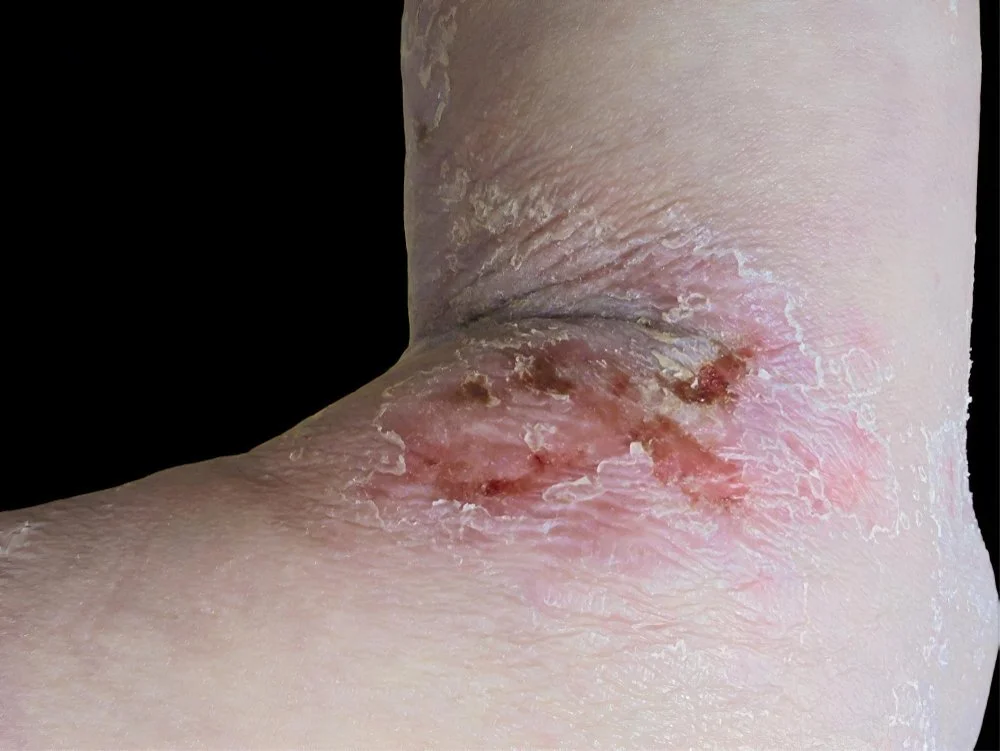
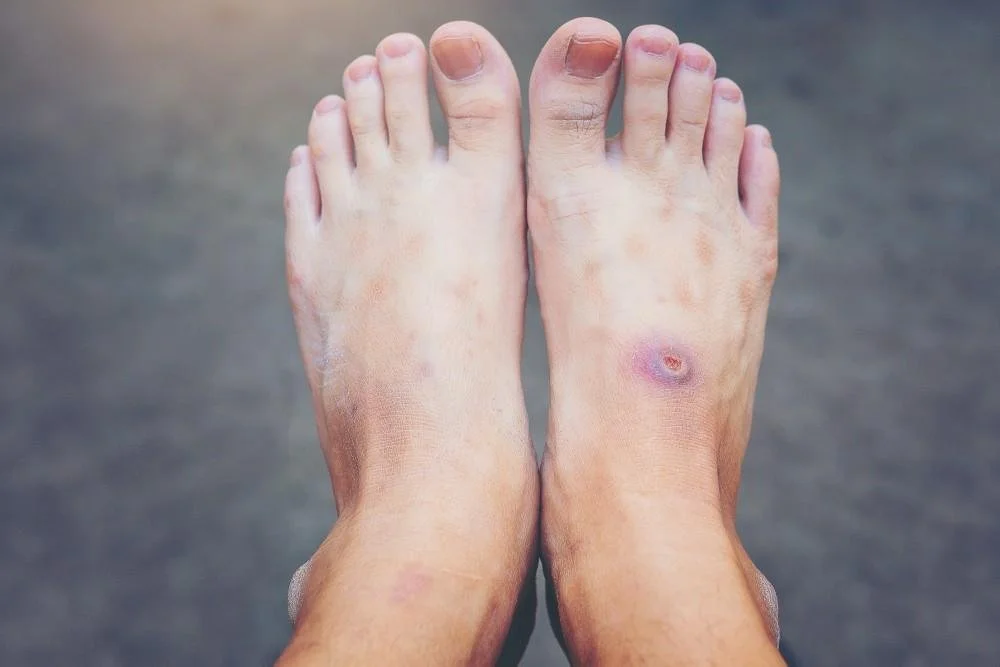
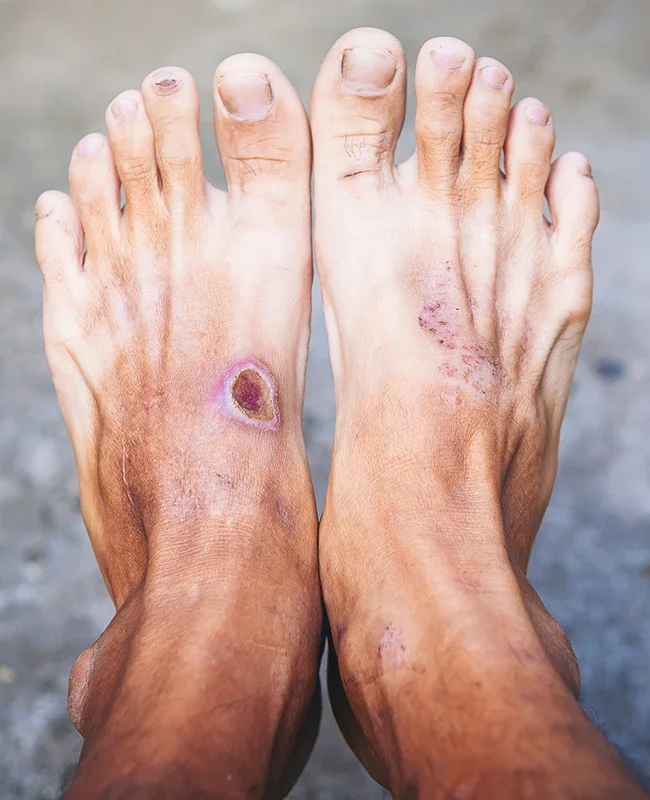
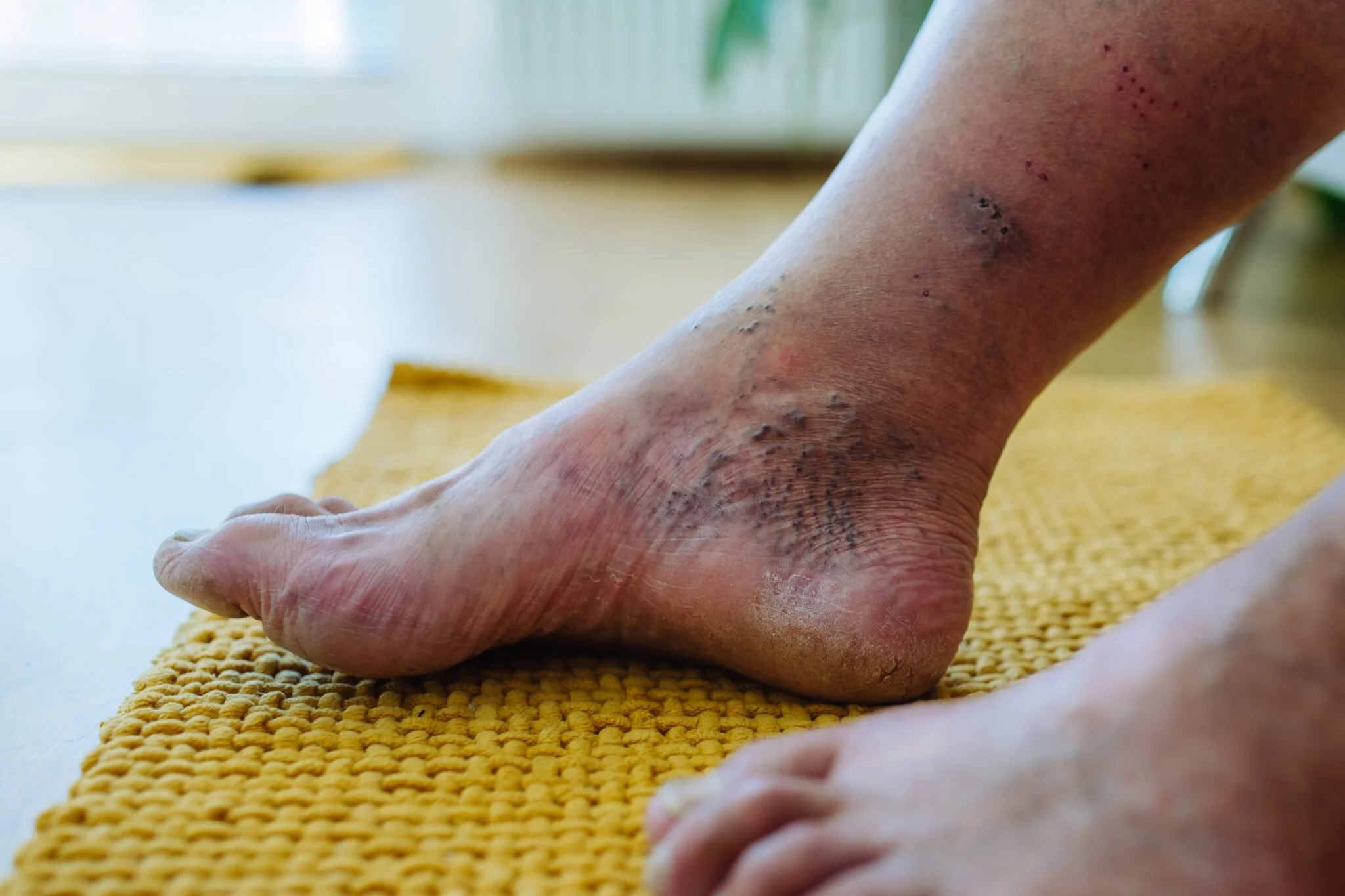
What is Diabetic Foot Care?
For individuals with diabetes, foot care is not a luxury—it is a preventative necessity. The condition often causes Peripheral Neuropathy, which is a loss of sensation that prevents a person from feeling a cut, blister, or even a foreign object in their shoe. Additionally, Peripheral Vascular Disease (poor circulation) slows the body's ability to deliver healing nutrients to the feet. Diabetic foot care involves routine clinical maintenance of toenails and skin, paired with a comprehensive neurovascular assessment to monitor for changes in sensation and blood flow. By having a foot specialist manage these tasks, patients reduce the risk of "bathroom surgery" accidents that could lead to non-healing ulcers or even amputation.
What can cause Diabetic Foot Complications?
Uncontrolled Blood Sugar: Chronic high glucose levels damage the small capillaries and nerve endings in the feet.
Inability to Self-Manage: Physical limitations, such as poor eyesight or reduced flexibility, make it dangerous for patients to use sharp clippers on themselves.
Poor Circulation: Swelling and arterial insufficiency prevent the skin from repairing itself after minor friction or injury.
Structural Deformities: Bunions or hammertoes create high-pressure areas that, in a diabetic foot, are prone to breaking down into deep ulcers.
What are the symptoms of Diabetic Foot Issues?
Neuropathic Changes: Tingling, "pins and needles," or a complete loss of feeling that makes it impossible to detect pain.
Trophic Changes: Skin that becomes thin, shiny, and hairless, or nails that become excessively thick and brittle (Onychogryphosis).
Delayed Healing: A simple scratch or blister that does not show signs of healing after several days.
Temperature Shifts: Feet that feel abnormally cold or, conversely, localized "hot spots" that indicate underlying infection or inflammation.
How do you treat the Diabetic Foot?
At Active Arches, we provide a sterile, clinical environment for routine maintenance:
Professional Maintenance: We perform routine nail trimming and the safe removal of hard skin and corns using medical-grade instruments. This is typically scheduled every 6–12 weeks depending on the patient's needs.
Clinical Assessment: During every visit, we check for pulses and test for "protective sensation" using specialized tools like the 10g monofilament.
Pressure Redistribution: We utilize Custom Orthotics and specialized footwear to offload high-pressure areas, significantly reducing the risk of ulcer formation.
Infection Control: We provide immediate treatment for ingrown nails or fungal infections before they can breach the skin barrier.
How can I prevent Diabetic Foot complications?
Prevention is a daily commitment. Patients should check their feet every single night using a mirror to look for redness or breaks in the skin. Maintaining stable blood sugar levels through diet and medication is the most effective way to protect your nerves. Always wear shoes—even indoors—to protect against accidental injury, and never attempt to cut out corns or calluses at home. Regular visits to a foot specialist ensure that your "foundation" is monitored by a professional who can catch potential problems long before you feel them.
Stop managing discomfort and start your recovery.
Book an appointment today and get a comprehensive assessment.
