Foot Arthritis
Rheumatoid Arthritis is a chronic autoimmune disease characterized by joint inflammation. Unlike osteoarthritis, which is caused by mechanical wear and tear, RA is a progressive condition where the immune system mistakenly attacks healthy joint tissue. The small joints of the feet and ankles are often among the first areas affected, leading to a cycle of inflammation, stiffness, and eventual joint deformity.
Rheumatoid Arthritis and Osteoarthritis
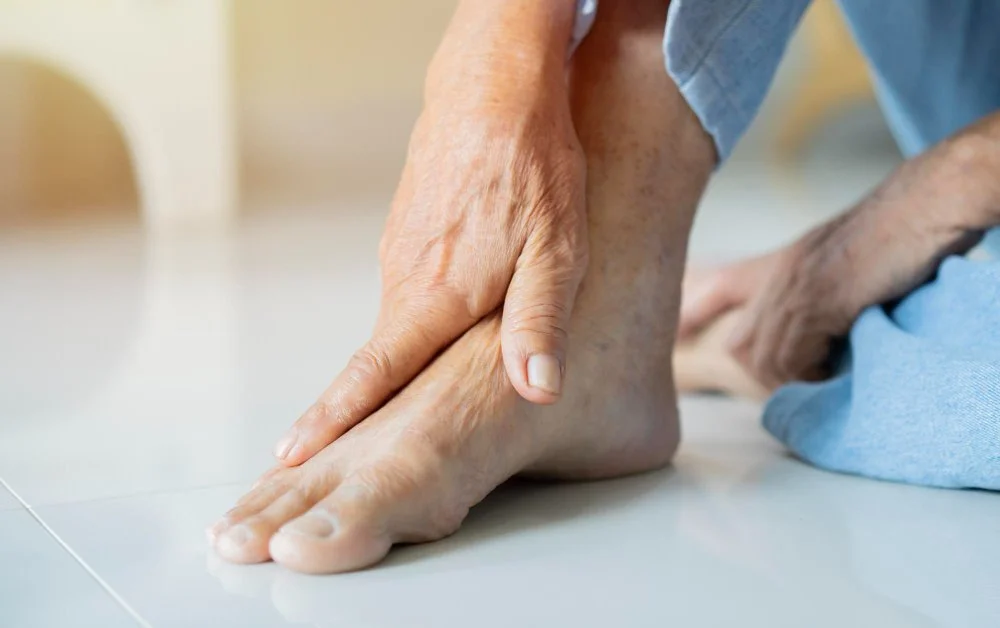

Symptoms
Joint pain and swelling; intense morning stiffness; warmth and redness around the joints; unexplained fatigue or low-grade fever; and the development of bunions or hammertoes.
Treatment
Custom Orthotics, Medical Foot Care, Orthopedic Footwear, Active Rehabilitation, Anti-inflammatory Medication, Anti-Rheumatic (DMARD) Therapy.
What is Foot Arthritis?
In a healthy foot, your joints are cushioned by cartilage and lubricated by a thin layer of fluid produced by the synovium. When arthritis sets in, this system breaks down—but the "why" depends on the type of arthritis you have.
What is Rheumatoid Arthritis (RA)?
RA is an autoimmune condition. The immune system mistakenly targets the synovium, causing it to thicken and become inflamed. This triggers the production of hard mineral deposits (calcification) and the erosion of cartilage and bone. Because joints require movement to remain healthy, the resulting stiffness creates a "vicious cycle": lack of movement leads to muscle weakness, making the joints even more prone to injury.
What is Osteoarthritis (OA)?
Often called "wear-and-tear" arthritis, OA is primarily a mechanical issue. Over time, the protective cartilage that cushions the ends of your bones wears down. As the "shock absorber" disappears, bone rubs against bone. This friction leads to the development of bone spurs (osteophytes) and localized inflammation. While RA is a systemic disease affecting the whole body, OA is often localized to specific joints that have been overworked or previously injured.
What Causes Foot Arthritis?
The triggers for foot pain are a complex interplay between your biology and your lifestyle:
Genetics and Biology: Genetics are responsible for nearly half of RA cases. For OA, your inherited foot structure—such as having very high arches or flat feet—can determine how quickly your cartilage wears out.
Environmental Stressors: Smoking is a massive risk factor for RA. For OA, the "stressor" is often physical, such as years of high-impact sports or repetitive heavy lifting.
Past Injuries: A hallmark of Osteoarthritis is "Post-Traumatic OA." A severe ankle sprain or a broken toe from years ago can change the way a joint moves, leading to decay decades later.
Systemic Health: Chronic inflammation from obesity or even gum disease can exacerbate RA. In OA, carrying excess weight adds significant mechanical pressure to the small joints of the foot and ankle.
Identifying the Symptoms
While both conditions cause pain, they "behave" differently throughout the day:
Symmetrical vs. Asymmetrical: RA typically affects the same joints on both sides of the body simultaneously (e.g., both second toe joints). OA is often asymmetrical, affecting one foot or one specific joint more severely.
The Morning Routine: RA is famous for "morning stiffness" that can last for an hour or more, only improving after significant movement. OA stiffness is usually brief (less than 30 minutes) but tends to get worse at the end of a long day of standing.
Physical Changes: RA can cause the foot to "splay" or widen as ligaments weaken. OA usually presents as hard, bony enlargements or "knots" on the joints that are firm to the touch.
How We Treat Foot Arthritis at Active Arches
While there is no cure for arthritis, our clinical team focuses on halting progression and restoring your quality of life:
Custom Orthotics: For RA, we focus on soft "accommodation" to protect sensitive areas. For OA, we use "functional" orthotics to realign the foot, shifting weight away from worn-out cartilage to healthier parts of the joint.
Active Rehabilitation: Movement is medicine. We prescribe gentle exercises to "flush out" inflammatory markers in RA and strengthen the "natural shock absorbers" (muscles) around OA joints.
Orthopedic Footwear: Proper shoes with extra depth are essential. They accommodate the swelling of RA and provide the rigid support needed to prevent the painful "hinging" of an osteoarthritic big toe.
Medical Foot Care: Because arthritis can make reaching your feet difficult, our Chiropodists provide professional maintenance for thickened nails and calluses, ensuring your skin remains healthy and ulcer-free.
Preventing Flares and Progression
Managing arthritis requires a proactive lifestyle. Staying active through low-impact exercises like swimming or yoga helps maintain joint lubrication without the "pounding" of running. Maintaining a healthy weight is the most effective way to reduce the mechanical stress on your feet, especially for Osteoarthritis.
Most importantly, early intervention is key. At the first sign of persistent joint warmth, "grinding" sensations, or morning stiffness, a consultation with a foot specialist can prevent minor wear from turning into permanent structural damage.
Stop managing discomfort and start your recovery.
Book an appointment today and get a comprehensive assessment.
